AAFP Questions
Infant Cough
Chlamydial pneumonia is usually seen in infants 3–16 weeks of age, and these patients frequently have been sick for several weeks. The infant appears nontoxic and is afebrile, but is tachypneic with a prominent cough. The physical examination will reveal diffuse crackles with few wheezes, and conjunctivitis is present in about 50% of cases. A chest film will show hyperinflation and diffuse interstitial or patchy infiltrates. Staphylococcal pneumonia has a sudden onset. The infant appears very ill and has a fever, and initially may have an expiratory wheeze simulating bronchiolitis. Signs of abdominal distress, tachypnea, dyspnea, and localized or diffuse bronchopneumonia or lobar disease may be present. The WBC count will show a prominent leukocytosis. Respiratory syncytial virus infections start with rhinorrhea and pharyngitis, followed in 1–3 days by a cough and wheezing. Auscultation of the lungs will reveal diffuse rhonchi, fine crackles, and wheezes, but the chest film is often normal. If the illness progresses, coughing and wheezing increase, air hunger and intercostal retractions develop, and evidence of hyperexpansion of the chest is seen. In some infants the course of the illness may be similar to that of pneumonia. Rash or conjunctivitis may occur occasionally, and fever is an inconsistent sign. The WBC count will be normal or elevated, and the differential may be normal or shifted either to the right or left. Chlamydial infections can be differentiated from respiratory syncytial virus infections by a history of conjunctivitis, the subacute onset and absence of fever, and the mild wheezing. There may also be eosinophilia. Parainfluenza virus infection presents with typical cold symptoms. Eight percent of infections affect the upper respiratory tract. In children hospitalized for severe respiratory illness, parainfluenza viruses account for about 50% of the cases of laryngotracheitis and about 15% each of the cases of bronchitis, bronchiolitis, and pneumonia.
Radial Head Subluxation
Radial head subluxation, or nursemaid’s elbow, is the most common orthopedic condition of the elbow in children 1–4 years of age, although it can be encountered before 1 year of age and in children as old as 9 years of age. The mechanism of injury is partial displacement of the radial head when the child’s arm undergoes axial traction while in a pronated and fully extended position. The classic history includes a caregiver picking up (or pulling) a toddler by the arm. In half of all cases, however, no inciting event is recalled.
Symptoms: When she returned the toddler was playing with toys using only her right arm, and was holding the left arm slightly pronated, flexed, and close to her body.
As long as there are no outward signs of fracture or abuse it is considered safe and appropriate to attempt reduction of the radial head before moving on to imaging studies. With the child’s elbow in 90° of flexion, the hand is fully supinated by the examiner and the elbow is then brought into full flexion. Usually the child will begin to use the affected arm again within a couple of minutes. If ecchymosis, significant swelling, or pain away from the joint is present, or if symptoms do not improve after attempts at reduction, then a plain radiograph is recommended.
erythema toxicum neonatorum
Usually resolves in the first week or two of life (SOR A). No testing is usually necessary because of the distinct appearance of the lesions. The cause is unknown.


Obesity terminology
The recommended terminology for weight classification in children is based on age and either BMI (for children ages 2–18 years) or weight-for-length ratio (for children ages 0–2 years). Children under the age of 2 years are identified as being overweight when their weight-for-length ratio exceeds the 95th percentile for their sex. The term obese is not used for children under the age of 2 years. Children age 2–18 years are appropriately classified as underweight when their BMI falls below the 5th percentile, healthy weight when their BMI is between the 5th and 85th percentile, overweight when their BMI is between the 85th and 94th percentile, and obese when their BMI is in the 95th or greater percentile. There is currently no standard definition of childhood morbid obesity, but obesity is sometimes classified as severe or extreme when a child’s BMI is at the 99th percentile or greater.
RSV
Respiratory syncytial virus (RSV) is a common cause of respiratory tract infections in children. The infections are usually self-limited and are rarely associated with bacterial co-infection, but in very young infants, prematurely born infants, or those with pre-existing heart/lung conditions, the infection can be severe. In North America, RSV season is November to April. Treatment is primarily supportive, including a trial of bronchodilators, with continued use only if there is an immediate response. Corticosteroids and antibiotics are not routinely indicated (SOR B). Routine laboratory and radiologic studies should not be used in making the diagnosis, as it is based on the history and physical examination (SOR C).
Children and Pneumonia
Amoxicillin is the recommended first-line treatment for previously healthy infants and school-age children with mild to moderate community-acquired pneumonia (CAP) (strong recommendation; moderate-quality evidence). The most prominent bacterial pathogen in CAP in this age group is Streptococcus pneumoniae, and amoxicillin provides coverage against this organism. Azithromycin would be an appropriate choice in an older child because Mycoplasma pneumoniae would be more common. Moxifloxacin should not be used in children. Ceftriaxone and cefdinir can both be used to treat CAP, but they are broader spectrum antibiotics and would not be a first-line choice in this age group.
Nondisplaced midshaft fracture
When compared to a figure-of-eight dressing, a sling has been shown to have similar fracture healing rates in patients with a nondisplaced midshaft clavicular fracture. In addition, a figure-of-eight dressing is uncomfortable and difficult to adjust, and patients have reported increased satisfaction when treated with a sling. Long and short arm casts are not appropriate options to manage a patient with a clavicular fracture. Operative treatment is an option to treat displaced midshaft fractures (SOR B). It should be noted that a Cochrane review of interventions for clavicle fracture pointed out that the studies of this problem were done in the 1980s and did not meet current standards. One of the conclusions of this review was that further research should be done.

Hip Labral Tear
Hip labral tear: This causes dull or sharp groin pain, which in some patients radiates to the lateral hip, anterior thigh, or buttock. The pain usually has an insidious onset, but occasionally begins acutely after a traumatic event. Half of patients also have mechanical symptoms, such as catching or painful clicking with activity. The FADIR and FABER tests are effective for detecting intra-articular pathology (the sensitivity is 75%–96% for the FADIR test and 88% for the FABER test), although neither test has high specificity. Magnetic resonance arthrography is considered the diagnostic test of choice for labral tears, as it has a sensitivity of 90% and an accuracy of 91%.
Trochanteric bursitis typically causes lateral hip pain with point tenderness over the greater trochanter of the femur.


Salmonella Treatment
The recommended management for patients who have non-severe Salmonella infection and are otherwise healthy is no treatment. Patients with high-risk conditions that predispose to bacteremia, and those with severe diarrhea, fever, and systemic toxicity or positive blood cultures should be treated with levofloxacin, 500 mg once daily for 7–10 days (or another fluoroquinolone in an equivalent dosage), or with a slow intravenous infusion of ceftriaxone, 1–2 g once daily for 7–10 days (14 days in patients with immunosuppression).
Vaccine and Seizures
Of the vaccines listed, the only one likely to put the child at risk for a seizure up to 2 weeks after administration is the MMR vaccine. Specifically, it is the measles component of the vaccine that is the potential culprit. A temperature of 39.4°C (103°F) or higher develops in approximately 5%–15% of susceptible vaccine recipients, usually 6–12 days after receipt of MMR vaccine. The fever generally lasts 1–2 days but may last up to 5 days.
Elbow Injuries
This patient has injured his ulnar collateral ligament (UCL). The UCL is the primary restraint to valgus stress on the elbow during overhead throwing. These injuries often occur in athletes participating in sports that require overhead throwing, such as baseball, javelin, and volleyball. Patients often report a pop followed by immediate pain and bruising around the medial elbow. The moving valgus stress test has 100% sensitivity and 75% specificity for diagnosing UCL injuries.
Medial epicondylitis usually presents with an insidious onset of pain related to a recent increase in occupational or recreational activities. Patients also often report weakened grip strength. The point of maximal tenderness is 5–10 mm distal to and anterior to the medial epicondyle. It is most often a tendinopathy of the flexor carpi radialis and the pronator teres.
Biceps tendinopathy usually presents with a history of vague anterior elbow pain and a history of repeated elbow flexion with forearm supination and pronation, such as dumbbell curls. Resisted supination produces pain deep in the antecubital fossa.
Cubital tunnel syndrome is a neuropathy of the ulnar nerve caused by compression or traction as it passes through the cubital tunnel of the medial elbow. The onset of pain is more insidious than UCL injury, occurring with repetitive activity, and is usually accompanied by numbness and tingling in the ulnar border of the forearm and hand. If it has existed for some time, the intrinsic hand muscle may become weak.
Tendinopathy of the triceps insertion is more common in weight lifters or athletes who repetitively extend their elbows against resistance. Pain occurs at the posterior elbow with resisted extension, and tenderness is located over the triceps insertion.
Cow Milk and Infants
Whole cow’s milk does not supply infants with enough vitamin E, iron, and essential fatty acids, and overburdens them with too much protein, sodium, and potassium. Skim and low-fat milk lead to the same problems as whole milk, and also fail to provide adequate calories for growth. For these reasons cow’s milk is not recommended for children under 12 months of age. Human breast milk or iron-fortified formula, with introduction of certain solid foods and juices after 4–6 months of age if desired, is appropriate for the first year of life.
OCP assessment
Before giving OCP, assess:
pregnancy
hypertension
Pap Screening
The U.S. Preventive Services Task Force recommends against screening for cervical cancer for women younger than 21, for women over the age of 65 who have had adequate screening in the recent past and are not at high risk, and for women who have had a hysterectomy with removal of the cervix and no history of CIN 2 or 3 or cervical cancer (USPSTF D recommendation). Women between the ages of 21 and 65 can be screened every 3 years with cytology alone, or the interval can be increased to 5 years after age 30 by using a combination of cytology and HPV testing (USPSTF A recommendation). The history of HPV vaccination is not a factor in screening decisions. Other organizations such as the American Cancer Society and the American College of Obstetricians and Gynecologists have similar guidelines.
DeQuervain
This patient has de Quervain’s tenosynovitis. Finkelstein’s test has good sensitivity and specificity (SOR C) in patients with a negative grind test. A positive grind test would be more consistent with scaphoid fracture. A hand radiograph with secondary thumb spica splinting would be appropriate for a suspected scaphoid fracture, but the insidious onset as opposed to overt trauma makes this diagnosis unlikely in this case. A short arm cast is not indicated in de Quervain’s tenosynovitis but may be appropriate for forearm/wrist fractures.
case: A 37-year-old graphic designer presents to your office with a history of several months of radial wrist pain. She does not recall any specific trauma but notes that it hurts to hold a coffee cup. Finkelstein’s test is positive and a grind test is negative, and there is tenderness to palpation over the radial tubercle.
SAH Diagnosis
Early diagnosis of a nontraumatic subarachnoid hemorrhage is paramount for achieving a good outcome when a patient presents with a headache that is unusually severe and feels different than other headaches. Risk factors include smoking, hypertension, heavy alcohol use, and a family history of aneurysm or hemorrhagic stroke. The initial evaluation should consist of noncontrast CT of the head (SOR C). If it is negative or equivocal the next step would be to perform a lumbar puncture to determine whether or not the cerebrospinal fluid is xanthochromic. The absence of xanthochromia rules out subarachnoid hemorrhage (SOR C).
Protonix risks
Currently known risks include increased fractures of the hip, wrist, and spine (SOR B), community-acquired pneumonia (SOR B), Clostridium difficile and other enteric infections (SOR C), hypomagnesemia (SOR B), and cardiac events when coadministered with clopidogrel (SOR B). PPIs may also affect the absorption of vitamins and minerals, including iron, vitamin B12, and folate (SOR C). There is no known association of PPIs with nephrolithiasis or urinary tract infections.
Hemochromatosis Diagnosis
The diagnosis of hereditary hemochromatosis requires a random measurement of serum ferritin and calculation of transferrin saturation. The transferrin saturation is calculated by dividing the serum iron level by the total iron binding capacity. If the serum ferritin level is elevated (>200 ng/mL in women) or the transferrin saturation is ³45% the HFE gene should be checked.
Copper vs Progesterone IUD
Women with severe cirrhosis or liver cancer should not use the levonorgestrel-releasing IUD, and the copper T is preferred. Hormonal contraceptives in general should be avoided in women with severe liver disease, as there is a known association between oral contraceptive use and the growth of hepatocellular adenoma, and this risk is thought to extend to other types of hormonal contraceptives (SOR C). Breast cancer is another contraindication to use of the levonorgestrel-releasing IUD, and the copper T would be preferred.
There is no difference in risk between the copper T and levonorgestrel-releasing IUD with regard to deep vein thrombosis/pulmonary embolism. However, the IUD is preferable to contraceptives containing estrogen.
IUDs can be used in nulliparous women and either type may be used, although there is some evidence that there are fewer complications with the levonorgestrel-releasing IUD.
Smoking does not preclude the use of either type of IUD. Patients with heart failure may use either type of IUD as well. Women with controlled hypertension may use either form, but there is a slight risk from use of the levonorgestrel-releasing IUD in women with uncontrolled hypertension, although the benefits outweigh the risks.
Refusal to eat
It is estimated that 3%–10% of infants and toddlers refuse to eat, according to their caregivers. Unlike other feeding problems such as colic, this problem tends to persist without intervention. It is recommended that caregivers establish routines for healthy scheduled meals and snacks, and follow them consistently. Parents should control what, when, and where children are being fed, whereas children should control how much they eat at any given time in accordance with physiologic signals of hunger and fullness. No food or drinks other than water should be offered between meals or snacks. Food should not be offered as a reward or present. Parents can be reassured that a normal child will learn to eat enough to prevent starvation. If malnutrition does occur, a search for a physical or mental abnormality should be sought.
Neck Cysts
In children, neck masses usually fall into one of three categories: developmental, inflammatory/reactive, or neoplastic. The history and physical examination can help narrow the diagnosis, with location of the mass being particularly helpful.
Branchial cleft cysts make up approximately 20% of neck masses in children. They commonly present in late childhood or adulthood, when a previously unrecognized cyst becomes infected (after URI). They are most frequently found anterior to the sternocleidomastoid muscle, but can also be preauricular. Thyroglossal duct cysts are located in the midline over the hyoid bone. Frequently, they elevate when the patient swallows. Dermoid cysts are usually mobile, moving with the overlying skin. They can be located in the submental or midline region. Thyroid tumors are also usually located in the midline. Malignant masses are usually hard, irregular, nontender, and fixed.
Bite
Antibiotic prophylaxis should be used for high-risk bite wounds. Factors associated with a high risk include a bite on an extremity with underlying venous and/or lymphatic compromise, a bite involving the hand, a bite near or in a prosthetic joint, cat bites, crush injuries, delayed presentation, puncture wounds, underlying diabetes mellitus, and immunosuppression. A Cochrane review of nine trials showed no statistical difference in infection rates between prophylaxis and no treatment, except when the bite wound was on the hand. The role of tetanus and rabies prophylaxis should be considered on a case-by-case basis. The other factors listed do not influence whether or not an antibiotic should be prescribed (SOR B).
Medication Physiology in Elderly
The physiologic changes that accompany aging result in altered pharmacokinetics. In older persons there is a relative increase in body fat and a relative decrease in lean body mass, which causes increased distribution of fat-soluble drugs such as diazepam. This also increases the elimination half-life of such medications. The volume of distribution of water-soluble compounds such as digoxin is decreased in older patients, which means a smaller dose is required to reach a given target plasma concentration. There is also a predictable reduction in glomerular filtration rate and tubular secretion with aging, which causes decreased clearance of medications in the geriatric population. The absorption of drugs changes little with advancing age. All of these changes are important to consider when choosing dosages of medications for the older patient.
HF and NSAIDS
NSAIDs cause an elevation of blood pressure due to their salt and water retention properties. This effect can also lead to edema and worsen underlying heart failure. In addition, all NSAIDs can have a deleterious effect on kidney function and can worsen underlying chronic kidney disease, in addition to precipitating acute kidney injury. Celecoxib, ibuprofen, meloxicam, and diclofenac are associated with an increased risk of cardiovascular adverse effects and myocardial infarction, compared with placebo. However, naproxen has not been associated with an increased risk of myocardial infarction and is therefore preferred over other NSAIDs in patients with underlying coronary artery disease risk factors (SOR B).
HSP Treatment
This patient meets the clinical criteria for Henoch-Schönlein purpura (HSP), an immune-mediated vasculitis found commonly in children under the age of 10. The clinical triad of purpura, abdominal pain, and arthritis is classic.
Almost 95% of children with HSP spontaneously improve, so supportive therapy is the main intervention. Acetaminophen or ibuprofen can be used for the arthritic pain. However, ibuprofen should be avoided in those with abdominal pain or known renal involvement. Prednisone has been found to help in those with renal involvement or other complications of the disease such as significant abdominal pain, scrotal swelling, or severe joint pains (SOR B). However, it is not effective for preventing renal disease or reducing the severity of renal involvement, as was once thought (SOR A).
Recommendations
A “D” recommendation means the U.S. Preventive Services Task Force (USPSTF) recommends against the service. There is moderate or high certainty that the service has no net benefit or that the harms outweigh the benefits. An “I” recommendation means the USPSTF concludes that the evidence is lacking, of poor quality, or conflicting, and the balance of benefits and harms cannot be determined. A “C” recommendation means the USPSTF recommends selectively offering or providing this service to individual patients based on professional judgment and patient preferences. There is at least moderate certainty that the net benefit is small. A “B” recommendation means the USPSTF recommends the service. There is high certainty that the net benefit is moderate or there is moderate certainty that the net benefit is moderate to substantial. An “A” recommendation means the USPSTF recommends the service and there is high certainty that the net benefit is substantial. The highest levels of evidence and most recent evidence available are used by the USPSTF in making all of its recommendations.
Pregnancy and Nausea
Nearly 75% of pregnant women are affected by nausea and vomiting of pregnancy. Though dietary modifications are often recommended, there is little evidence to support their use. Vitamin B6 is recommended as first-line therapy. It is safe to use in the first trimester and is associated with less drowsiness compared with other medications.
Methimazole SE
Approximately 0.3% of patients taking methimazole develop agranulocytosis, usually within the first 60 days of starting therapy. Other rare complications of methimazole include serum sickness, cholestatic jaundice, alopecia, nephrotic syndrome, hypoglycemia, and loss of taste. It is associated with an increased risk of fetal anomalies, so propylthiouracil (PTU) is preferred in pregnancy. The other medications listed are not known to cause the combination of agranulocytosis and cholestatic jaundice that this patient has.
Gestational DM
These include a decreased risk for operative delivery, large-for-gestational-age infants, shoulder dystocia, and maternal preeclampsia. Although a significant percentage of women with GDM subsequently develop type 2 diabetes mellitus after delivery, pharmacologic treatment of GDM has not been shown to decrease that risk. In addition, neither perinatal death nor the likelihood of small-for-gestational-age infants is significantly affected. The risk of neonatal hypoglycemia has also not consistently been shown to be affected by treatment.
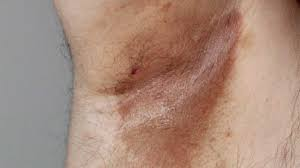
Erythramas
All of the diagnoses listed are intertriginous rashes but only erythrasma fluoresces with Wood’s light. Erythrasma is a superficial gram-positive bacterial infection caused by Corynebacterium minutissimum. The fluorescence is caused by porphyrins. Erythrasma is most often seen between the toe web spaces, followed by the groin and axillae. There are multiple treatments, including topical and oral erythromycins and clindamycins (level of evidence 3, strength of evidence 1).

Postpartum Hemorrhage
Carboprost (Hemabate), Methylergonovine, Misoprostol (Cytotec), Oxytocin (Pitocin)
All of the drugs listed are appropriate for uterine atony and postpartum hemorrhage. Carboprost should not be used in this patient, however, as it is contraindicated in patients with asthma. Methylergonovine is contraindicated in hypertensive patients but may be used in patients with asthma.
Acute Parotitis
This case is typical for acute parotitis, which is commonly caused by dehydration and can be diagnosed from the history and examination. Empiric treatment is directed toward gram-positive and anaerobic organisms (amoxiciliin/clavunata), with the most common pathogen being Staphylococcus. These are often penicillin resistant so a β-lactamase inhibitor is the agent of choice. Treatment should be followed up with cultures. Administration of sialagogues such as lemon drops may be helpful, as well as parotid gland massage.
CT or MRI may help confirm the diagnosis but imaging is usually not necessary. The history and clinical examination are most important for making the diagnosis. Incision and drainage would be appropriate only for an abscess, and surgical removal of the parotid gland is not indicated.
Infant Fever
Any child younger than 29 days old with a fever and any child who appears toxic, regardless of age, should undergo a complete sepsis workup and be admitted to the hospital for observation until culture results are known or the source of the fever is found and treated.
Observation only, with close follow-up, is recommended for nontoxic infants 3–36 months of age with a temperature <39.0°C (102.2°F). Children 29–90 days old who appear to be nontoxic and have negative screening laboratory studies, including a CBC and urinalysis, can be sent home with precautions and with follow-up in 24 hours. Testing for neonatal herpes simplex virus infection should be considered in patients with risk factors, including maternal infection at the time of delivery, use of fetal scalp electrodes, vaginal delivery, cerebrospinal fluid pleocytosis, or herpetic lesions. Testing also should be considered when a child does not respond to antibiotics.
Cervical Lymphadenitis
This child has cervical lymphadenitis, characterized by systemic symptoms, unilateral lymphadenopathy, skin erythema, node tenderness, and a node that is 2–3 cm in size. The most common organisms associated with lymphadenitis are Staphylococcus aureus and group A Streptococcus. Empiric antibiotic therapy with observation for 4 weeks is acceptable for children with presumed reactive lymphadenopathy (SOR C). If symptoms do not resolve, or if the mass increases in size during antibiotic treatment, further evaluation is appropriate.
When imaging is indicated, ultrasonography is the preferred initial study for most children with a neck mass. CT with intravenous contrast media is the preferred study for evaluating a malignancy or a suspected retropharyngeal or deep neck abscess that may require surgical drainage. If the initial mass is suspicious for malignancy (>3.0 cm in size, hard, firm, immobile, and accompanied by type B symptoms such as fever, malaise, weight loss, or night sweats) immediate referral to a surgeon for evaluation and possible biopsy is appropriate.
Trench Fever
Lice, scabies, and secondary bacterial infections are endemic in the homeless. Body lice transmit Bartonella quintana, which causes trench fever. This disease got its name in World War I, when soldiers in the trenches were often infested with body lice. This is a serious disease that can be treated with antibiotics.
Otitis Media
The usual treatment for AOM is amoxicillin, but an antibiotic with additional B-lactamase coverage, such as amoxicillin/clavulanate, should be given if the child has received amoxicillin within the past 30 days, has concurrent purulent conjunctivitis, or has a history of AOM unresponsive to amoxicillin (SOR C). Penicillin-allergic patients should be treated with an alternative antibiotic such as cefdinir, cefuroxime, cefpodoxime, or ceftriaxone.
Breastmilk feeding
Although breast milk is the ideal source of nutrition for healthy term infants, supplementation with 400 IU/day of vitamin D is recommended beginning in the first few days of life and continuing until the child is consuming at least 500 mL/day of formula or milk containing vitamin D (SOR B). The purpose of supplementation is to prevent rickets. Unless the baby is anemic or has other deficiencies, neither iron nor a multivitamin is necessary at this age. For exclusively breastfed infants, iron supplementation should begin at 4 months of age. Parents often mistakenly think babies need additional water, which can be harmful because it decreases milk intake and can cause electrolyte disturbances. The introduction of cereal is recommended at 6 months of age.
Child Bone Fractures
Posterior or posteromedial rib fractures are secondary to child abuse until proven otherwise, justifying notification of Child Protective Services or referral to an emergency department familiar with the appropriate workup. Osteogenesis imperfecta can cause continuous beading of the ribs and crumpled long bones such as accordina femora, and is often associated with blue sclerae, skin fragility, or brittle teeth. A skeletal survey is appropriate in a child 2 years of age or younger suspected of being physically abused. It is not thought to be necessary in children 4 years of age or older, especially in a case where suspicious fractures have already been discovered. Rickets usually is associated with long bone bowing deformities. In the chest it can cause prominence of the costochondral junctions (rachitic rosary) and indentation of the lower ribs where the diaphragm attaches (Harrison’s grooves).
Gestational Hypertension and Induction
The 2013 ACOG guideline recommends induction of labor for gestational hypertension after 37 weeks.
Pregnancy Screening
All pregnant women should be screened for asymptomatic bacteriuria between 11 and 16 weeks gestation and should be appropriately treated if the urine culture is positive. Asymptomatic bacteriuria is a known contributor to recurrent urinary tract infections, pyelonephritis, and preterm labor. TSH levels should be checked in patients with a history of thyroid disease or symptoms of disease, but universal testing is not recommended. Although treatment of bacterial vaginosis decreases the risk of low birth weight and premature rupture of membranes, universal screening is not recommended. This patient should be screened for both group B Streptococcus (GBS) and diabetes mellitus, but not at this point in her pregnancy. GBS screening should be done between 35 and 37 weeks gestation, and diabetes screening should be performed with a 50-g glucose load between 24 and 28 weeks gestation.
Hematospermia
In males younger than 40, hematospermia is usually benign and self-limited. Examination of the testes and prostate is warranted but findings are usually normal. If the patient is sexually active a screen for STDs is reasonable. Imaging of the genitourinary tract, a serum PSA level, and urology referral are unnecessary in this age group unless the history or physical examination suggests an unusual cause.
Male Hypogonadism
The best initial test for the diagnosis of male hypogonadism is measurement of total testosterone in serum in a morning sample. Low concentrations of testosterone in serum should be confirmed by repeat measurement. If abnormalities in concentrations of sex hormone–binding globulin are suspected, measurement of free or bioavailable testosterone is indicated. Examples of conditions associated with altered sex hormone–binding globulin include liver disease, obesity, and diabetes mellitus.
Preeclampsia Prevention
A 2013 update from the American College of Obstetricians and Gynecologists on hypertension in pregnancy summarizes the evidence regarding prevention of preeclampsia. The only medication with sufficient evidence to support its routine use is aspirin at dosages of 60–80 mg daily. In a high-risk population, defined as women with a history of preeclampsia in two or more pregnancies or a history of preeclampsia with delivery at <34 weeks, the risk of preeclampsia is sufficiently high to justify the use of aspirin, with a number needed to treat of 50 to prevent one case of preeclampsia.
Pain Meds and ESRD
Fentanyl is one of the preferred narcotics in patients with end-stage renal disease. Fentanyl’s elimination is 99% hepatic and it has a long history of safe use in patients with renal failure. Morphine, hydromorphone, and hydrocodone can be used in these patients, but these drugs require close monitoring for side effects and indications for dosage reduction because they have active metabolites that accumulate in patients with renal failure. Meperidine, codeine, and propoxyphene are all contraindicated in chronic kidney disease because of the accumulation of toxic metabolites.
Aseptic Olecranon Bursitis
Aseptic olecranon bursitis is often preceded by minor trauma to the elbow followed by a nontender, boggy mass over the olecranon. Septic olecranon bursitis causes not just swelling, but also erythema, warmth, and pain. Half of affected individuals will have a fever. If septic bursitis is suspected, aspiration with bursal fluid analysis should be done and antibiotic therapy should be initiated. Aspiration is not recommended for the initial treatment of aseptic bursitis, as complications such as infection may occur. Management initially is with ice, compression dressings, and avoidance of activities that aggravate the problem. If conservative therapy is unsuccessful the problem can be managed by aspiration followed by compression dressings for 2 weeks. The bursa may be injected with a corticosteroid, but this could cause skin atrophy or infection. Surgical bursectomy can be offered for refractory cases lasting over 3 months.
Hemochromatosis
The diagnosis of hereditary hemochromatosis requires a random measurement of serum ferritin and calculation of transferrin saturation. The transferrin saturation is calculated by dividing the serum iron level by the total iron binding capacity. If the serum ferritin level is elevated (>200 ng/mL in women) or the transferrin saturation is ³45% the HFE gene should be checked. Measurement of liver transaminases plays a role in determining liver disease but is not helpful in the diagnosis.
Pre op drugs
If recommended prior to surgery, β-blockers should be started several weeks beforehand and carefully titrated. They may be harmful if initiated in the immediate perioperative period. Statins are recommended in the perioperative period for vascular surgery regardless of other cardiac risk factors; a statin would ideally have been initiated previously in this case, but may still be started in the immediate preprocedural period.
Low dose CT
The U.S. Preventive Services Task Force (USPSTF) recommends screening smokers for lung cancer with low-dose CT. Patients should be age 55–80 and healthy. They should be current smokers or have quit within the past 15 years, and have a 30-pack-year history of smoking. The screening test is low-dose CT of the chest.
Hyponatremia
The initial treatment for mild euvolemic hyponatremia is fluid restriction. Intravenous isotonic saline would be indicated for mild hypovolemic hyponatremia. Intravenous hypertonic saline would be indicated for severe hyponatremia with symptoms. Intravenous diuretics would be indicated for hypervolemic hyponatremia, such as in heart failure, along with fluid and sodium restriction.
Hep B Screening
The CDC recommends screening for hepatitis B in patients on hemodialysis, household contacts of individuals with chronic hepatitis B, patients on immunosuppressive therapy, and all pregnant women. Other individuals who should be screened include anyone exposed to bodily fluids of infected individuals, such as sexual partners or infants of infected mothers. Behavioral risks such as intravenous drug use are also an indication for screening. Patients from areas where HBsAg prevalence is >2% should also be screened.
Varus/Valgus in Children
This case is consistent with physiologic genu valgus, and the parents should be reassured. Toddlers under 2 years of age typically have a varus angle at the knee (bowlegs). This transitions to physiologic genu valgus, which gradually normalizes by around 6 years of age.
Allergies antihistamines vs glucocorticoids
Azelastine, an intranasal antihistamine, is effective for controlling symptoms but can cause somnolence and a bitter taste. Oral antihistamines are not as useful for congestion as for sneezing, pruritus, and rhinorrhea. Overall, they are not as effective as topical glucocorticoids for allergic rhinitis.
Pain in big toe
The first metatarsophalangeal (MTP) joint has two sesamoid bones, and injuries to these bones account for 12% of big-toe injuries. Overuse, a sharp blow, and sudden dorsiflexion are the most common mechanisms of injury.
Morton’s neuroma typically causes numbness involving the digital nerve in the area, and usually is caused by the nerve being pinched between metatarsal heads in the center of the foot.
Acute Epididymitis
In sexually active men under age 35, acute epididymitis is caused most frequently by Chlamydia trachomatis and less commonly by Neisseria gonorrhoeae. Clinical features suggestive of urethritis may be absent (subclinical urethritis). Epididymitis in men who have practiced unprotected insertive rectal intercourse is often caused by Enterobacteriaceae.
Compartment Syndrome
Before the classic findings develop, patients will have tenderness out of proportion to the physical appearance of the injury and, most importantly, severe pain in the involved compartment with passive stretching of the involved muscles.
CCB Ingestion
Substantial toxicity can occur with one or two tablets, and all children suspected of ingesting a calcium channel blocker should be admitted to a pediatric intensive-care unit for monitoring and management.
The use of gastric emptying, cathartics, or adsorptive agents is unlikely to be helpful and should be considered only in patients presenting within 1 hour of ingestion, if then. The American Academy of Pediatrics has advised that syrup of ipecac not be kept in the home because of toxicity and dubious benefit.
Osteoporosis Screening
All women ≥65 (SOR A) and all men ≥70 (SOR C) should be screened for osteoporosis. For men and women age 50–69, the presence of factors associated with low bone density would merit screening. Risk factors include low body weight, previous fracture, a family history of osteoporosis with fracture, a history of falls, physical inactivity, low vitamin D or calcium intake, and the use of certain medications or the presence of certain medical conditions.
Chronic systemic diseases that increase risk include COPD, HIV, severe liver disease, renal failure, systemic lupus erythematosus, and rheumatoid arthritis. Endocrine disorders that increase risk include type 1 diabetes mellitus, hyperparathyroidism, hyperthyroidism, Cushing’s syndrome, and others. Medications that increase risk include anticonvulsants, corticosteroids, and immunosuppressants. Nutritional risks include celiac disease, vitamin D deficiency, anorexia nervosa, gastric bypass, and increased alcohol or caffeine intake.
Shoulder Pain
Disease
PE
Frozen Shoulder
Loss of active and passive
Rotator Cuff Tear
Passive intact, no pain
Impringement
Passive intact, pain
Men vs Women Physiology
There are key physiologic differences between women and men that can have important implications for drug activity. Gastrointestinal transit times are slower in women than in men, which can diminish the absorption of medications such as metoprolol, theophylline, and verapamil. In addition, women should wait longer after eating before taking medications that should be administered on an empty stomach, such as ampicillin, captopril, levothyroxine, loratadine, and tetracycline.
Women also secrete less gastric acid than men, so they may need to drink an acidic beverage to aid in absorption of medications that require an acidic environment, such as ketoconazole. Women usually have lower BMIs than men, and may need smaller loading or bolus dosages of medications to avoid unnecessary adverse reactions. Women typically have higher fat stores than men, so lipophilic drugs such as benzodiazepines and neuromuscular blockers have a longer duration of action. Women also have lower glomerular filtration rates than men, resulting in slower clearance of medications that are eliminated renally, such as digoxin and methotrexate.
Rosacea
Management includes avoidance of precipitating factors and use of sunscreen. Oral metronidazole, doxycycline, or tetracycline also can be used, especially if there are ocular symptoms. These are often ineffective for the flushing, so low-dose clonidine or a nonselective β-blocker may be added.
Topical treatments such as metronidazole and benzoyl peroxide may also be effective, particularly for mild cases.
Tendinopathy
The diagnosis of tendinopathy of the posterior tibial tendon is important, in that the tendon’s function is to perform plantar flexion of the foot, invert the foot, and stabilize the medial longitudinal arch. An injury can, over time, elongate the midfoot and hindfoot ligaments, causing a painful flatfoot deformity.
The patient usually recalls no trauma, although the injury may occur from twisting the foot by stepping in a hole. This is most commonly seen in women over the age of 40. Without proper treatment, progressive degeneration of the tendon can occur, ultimately leading to tendon rupture.
Pain and swelling of the tendon is often noted, and is misdiagnosed as a medial ankle sprain. With the patient standing on tiptoe, the heel should deviate in a varus alignment, but this does not occur on the involved side. A single-leg toe raise should reproduce the pain, and if the process has progressed, this maneuver indicates progression of the problem.
While treatment with acetaminophen or NSAIDs provides short-term pain relief, neither affects long-term outcome. Corticosteroid injection into the synovial sheath of the posterior tibial tendon is associated with a high rate of tendon rupture and is not recommended. The best initial treatment is immobilization in a cast boot or short leg cast for 2–3 weeks.
Pregnancy Bleeding
Late pregnancy bleeding may cause fetal morbidity and/or mortality as a result of uteroplacental insufficiency and/or premature birth. The condition described here is placental abruption (separation of the placenta from the uterine wall before delivery).
There are several causes of vaginal bleeding that can occur in late pregnancy that might have consequences for the mother, but not necessarily for the fetus, such as cervicitis, cervical polyps, or cervical cancer. Even advanced cervical cancer would be unlikely to cause the syndrome described here. The other conditions listed may bring harm to the fetus and/or the mother.
Uterine rupture usually occurs during active labor in women with a history of a previous cesarean section or with other predisposing factors, such as trauma or obstructed labor. Vaginal bleeding is an unreliable sign of uterine rupture and is present in only about 10% of cases. Fetal distress or demise is the most reliable presenting clinical symptom. Vasa previa (the velamentous insertion of the umbilical cord into the membranes in the lower uterine segment) is typically manifested by the onset of hemorrhage at the time of amniotomy or by spontaneous rupture of the membranes. There are no prior maternal symptoms of distress. The hemorrhage is actually fetal blood, and exsanguination can occur rapidly. Placenta previa (placental implantation that overlies or is within 2 cm of the internal cervical os) is clinically manifested as vaginal bleeding in the late second or third trimester, often after sexual intercourse. The bleeding is typically painless, unless labor or placental abruption occurs.
Chlaymydia Pneumonia
This infant has the typical findings of chlamydial pneumonia, which usually develops 1–3 months after birth and should be suspected in a young infant who has tachypnea, a staccato cough, and no fever (SOR A). Radiographs often show hyperinflation and infiltrates, and a CBC will reveal eosinophilia.
Lichen Planus
This patient has classic lichen planus, with pruritic, symmetrically distributed papular lesions. The violaceous flat-topped papules, usually 3–6 mm in size, are distinct and so characteristic in appearance that a biopsy is usually not necessary to make the diagnosis. First-line treatment is with high-potency topical corticosteroids such as clobetasol, as mid-potency topical agents such as triamcinolone are ineffective. Topical calcineurin inhibitors, including tacrolimus, can be used in cases not responding to topical corticosteroids. While scabies can masquerade as a variety of other dermatoses, retreatment with a scabicide is not indicated in this patient.

Hip Pain
Gradually worsening anterolateral hip joint pain that is sharply accentuated when pivoting laterally on the affected hip or moving from a seated to a standing position is consistent with femoroacetabular impingement. Reproduction of the pain on range-of-motion examination by manipulating the hip into a position of flexion, adduction, and internal rotation (FADIR test) is the most sensitive physical finding. Special radiographic imaging of the flexed and adducted hip can emphasize the anatomic abnormalities associated with impingement that may go unnoticed on standard radiographic series views. Although the pain associated with avascular necrosis is similarly insidious and heightened when bearing weight, tenderness is usually evident with hip motion in any direction. Osteoarthritis of the hip generally occurs in individuals of more advanced age than this patient, and the pain produced is typically localized to the groin area and can be elicited by flexion, abduction, and external rotation (FABER test) of the affected hip.Bursitis manifests as soreness after exercise and tenderness over the affected bursa.
Respiratory Secretion
Glycopyrrolate does not cross the blood-brain barrier, and is therefore least likely to cause central nervous system effects such as sedation. The other medications listed do cross the blood-brain barrier.
Atropine, Transdermal scopolamine (Transderm Scop), Hyoscyamine (Levsin)
Osler Weber Rendu
Pulmonary arteriovenous malformations are found in 15%–30% of patients with hereditary hemorrhagic telangiectasia (HHT), also known as Osler-Weber-Rendu syndrome. All patients with possible or confirmed HHT should be screened for pulmonary arteriovenous malformations with contrast echocardiography (SOR C). While contrast echocardiography is used to detect atrioseptal and ventricular septal defects, neither of these conditions is particularly prevalent in HHT. Aortic aneurysms and myocardial perfusion defects are also not associated with HHT.
Hep B Phases
Chronic hepatitis B has three major phases: immune-tolerant, immune-active, and inactive-carrier.There usually is a linear transition from one phase to the next, but reactivation from immune-carrier phase to immune-active phase also can be seen.
Active viral replication occurs during the immune-tolerant phase when there is little or no evidence of disease activity, and this can last for many years before progressing to the immune-active phase (evidenced by elevated liver enzymes, indicating liver inflammation, and the presence of HBeAg, indicating high levels of HBV DNA). Most patients with chronic hepatitis B eventually transition to the inactive-carrier phase, which is characterized by the clearance of HBeAg and the development of anti-HBeAg, accompanied by normalization of liver enzymes and greatly reduced levels of hepatitis B virus in the bloodstream.
Nephritic Abscess
Perinephric abscess is an elusive diagnostic problem that is defined as a collection of pus in the tissue surrounding the kidney, generally in the space enclosed by Gerota’s fascia. Mortality rates as high as 50% have been reported, usually from failure to diagnose the problem in a timely fashion. The difficulty in making the diagnosis can be attributed to the variable constellation of symptoms and the sometimes indolent course of this disease. The diagnosis should be considered when a patient has fever and persistence of flank pain even after appropriate antibiotics.
Most perinephric infections occur as an extension of an ascending urinary tract infection, commonly in association with renal calculi or urinary tract obstruction. Patients with anatomic urinary tract abnormalities or diabetes mellitus have an increased risk. Clinical features may be quite variable, and the most useful predictive factor in distinguishing uncomplicated pyelonephritis from perinephric abscess is persistence of fever for more than 4 days after initiation of antibiotic therapy. The radiologic study of choice is CT. This can detect perirenal fluid, enlargement of the psoas muscle (both are highly suggestive of the diagnosis), and perirenal gas (which is diagnostic). The sensitivity and specificity of CT is significantly greater than that of either ultrasonography or intravenous pyelography.
Drainage, either percutaneously or surgically, along with appropriate antibiotic coverage reduces both morbidity and mortality from this condition.
Perilymphatic Fistula
A perilymphatic fistula between the middle and inner ear may be caused by barotrauma from scuba diving, as well as by direct blows, heavy weight bearing, and excessive straining (e.g., with sneezing or bowel movements.) This patients recent trip involved two of these potential factors. Vestibular neuronitis is a more sudden, unremitting syndrome. Menieres disease is manifested by episodes of vertigo, associated with hearing loss and often with nausea and vomiting. Benign paroxysmal positional vertigo is more likely in older individuals, and is associated with postural change. Multiple sclerosis requires symptoms in multiple areas and is not thought to be provoked by climate change.
Female Triad
“Disordered eating” has been replaced by a spectrum ranging from “optimal energy availability” to “low energy availability with or without an eating disorder”
“Amenorrhea” has been replaced by a spectrum ranging from “eumenorrhea” to “functional hypothalamic amenorrhea”
“Osteoporosis” has been replaced by a spectrum ranging from “optimal bone health” to “osteoporosis”
Persistent AOM
Streptococcus pneumoniae, Haemophilus influenzae, and Moraxella catarrhalis are the most common bacterial isolates from the middle ear fluid of children with acute otitis media. Penicillin-resistant S. pneumoniae is the most common cause of recurrent and persistent acute otitis media.
Fundal Height
Fundal height should be measured at each prenatal visit from 24-38 weeks gestation. This provides a rough estimate of fetal growth.
If fundal height is more than 3 cm above or below the expected value (gestational age in weeks), this is suggestive of an abnormality of fetal growth or amniotic fluid volume. If the fundal height is at least 3 cm below the expected value for gestational age, an ultrasound should be ordered to determine if the fetus is small for dates, or suffers from intrauterine growth restriction. However, it is important to remember that abnormalities of amniotic fluid such as oligohydramnios can also lead to a fundal height that is less than expected for gestational age.
Pulmonary Nodules
adiographic features of benign nodules include a diameter less than 5 mm, a smooth border, a solid appearance, concentric calcification, and a doubling time of less than 1 month or more than 1 year. Features of malignant nodules include a size >10 mm, an irregular border, a “ground glass” appearance, either no calcification or an eccentric calcification, and a doubling time of 1 month to 1 year (SOR B).
Last updated